The Permission Slip Trap: Decoding Prior Authorizations
- Mar 16
- 3 min read
Imagine your doctor determines exactly what medication you need to stay healthy, writes the prescription, and sends it to the pharmacy, only for a middleman to step in and say, "Not so fast." This is Prior Authorization, or PA for short—a requirement that your doctor must obtain "permission" from your Pharmacy Benefit Manager (PBM) before your medicine will be covered. While PBMs frame this as a safety or cost-saving measure, 93% of physicians report that these requirements routinely delay access to necessary medical care (American Medical Association Survey 2024).

A Major Burden with High Stakes
For many patients, the prior authorization process is not just a minor inconvenience; it is a significant barrier to health. According to a Kaiser Family Foundation Health Tracking Poll, approximately 7 in 10 insured adults (69%) describe prior authorization as a burden to receiving care. Even more telling is that 32% rank it as a "major burden", which patients find more difficult than understanding a medical bill (23%) or finding a doctor who accepts their insurance (17%).
The consequences of this "permission slip" system are often dangerous. The American Medical Association (AMA) reports that 82% of physicians have seen patients completely abandon their prescribed treatment because the prior authorization process was too difficult or took too long. When treatment is abandoned, the PBM "wins" by avoiding the cost of the medication, but the patient loses their path to recovery. This is a direct safety issue. One in four physicians (24%) reports that PA delays have led to serious adverse events for their patients, including hospitalization or permanent impairment.
Has a Prior Authorization Ever Been an Issue for You?
Yes
No
The Tennessee Reality: The Caremark Audit
The impact of these gatekeepers is felt acutely in Tennessee, where recent investigations have pulled back the curtain on how these systems truly operate. In February 2026, the Tennessee Department of Commerce and Insurance (TDCI) released a staggering audit of CVS Caremark’s 2024 operations, which resulted in $750,000 in penalties for repeated violations.
The audit revealed that the system is frequently tilted against both patients and local pharmacies. Specifically, it found that Caremark denied nearly 28% of appeals without giving providers the legally required time to submit necessary clinical information. In 53% of approved appeals, Caremark failed to provide the necessary instructions for pharmacies to receive their correct payment, creating massive price gaps that threaten the survival of local pharmacies.
Framing the Strategy: Cost-Control vs. Clinical Care
It is vital to understand that Prior Authorization is primarily a cost-control tactic, not a clinical review. By creating an administrative process that is "overwhelming by design," PBMs bank on the exhaustion of patients and doctors. They are betting that the hours spent on hold and the repetitive paperwork will cause you to quit before the medicine is ever approved.
When a middleman systematically ignores appeal rules and creates such massive barriers to care, it isn't just a "business issue"—it's a direct threat to the healthcare access of everyone who relies on a medication. However, you do not have to be the one who "blinks" first. While the initial "no" can be disheartening, data shows that over 80% of denials are eventually overturned on appeal. Knowledge of your rights is your best defense against this "permission slip" trap.
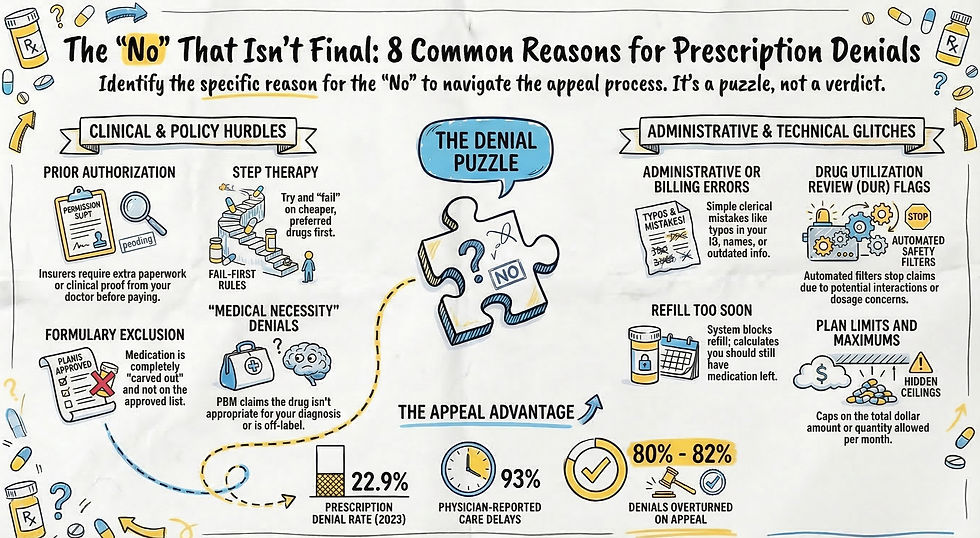
If you want to discover the specific justifications PBMs use to issue these rejections, read The “No” That Isn’t Final for a breakdown of the most common reasons for prescription denials. To learn how to move from being a victim of this system to a master of it, explore Beyond the Rejection: Power Moves for Overcoming Denials.



Comments