The Gatekeepers: What are PBMs and Why Do They Control Your Medicine?
- Mar 16
- 3 min read
The plain white envelope arrives in your mailbox, looking deceptively ordinary, but its contents feel incredibly heavy. You open it to find a single word standing between you and your health: Denied. For most, this feels like a definitive end, a bureaucratic stone wall blocking access to life-sustaining treatment.
But here is the industry’s open secret: this system is "overwhelming by design". Health insurance giants and their middlemen are betting that the hours spent on hold, the confusing jargon, and the sheer fatigue of the process will cause you to quit. In this high-stakes environment, you are not just a patient; you are an auditioning performer waiting for a callback from an invisible director you will never meet. That director is your Pharmacy Benefit Manager (PBM).
The "Bouncers" of Healthcare
Originally created in the 1960s to process claims, PBMs have evolved into the "bouncers" of the healthcare world. They act as the unseen gatekeepers between your doctor's prescription pad and your pharmacy. Their decisions dictate exactly which drugs are covered, what your co-pay will be, and which pharmacies are allowed in your network.
The market is dominated by a powerful "Big Three"—CVS Caremark, Express Scripts, and OptumRx, which together control roughly 80% of all prescriptions for about 275 million Americans. Because these three companies hold so much power, they have incredible leverage over which drugs make it to the shelf and at what price.
The Conflict of Interest: Vertical Integration
To understand why the "Big Three" exert such total control, it is essential to look at their vertical integration, where a single parent company owns every stage of the healthcare pipeline. This "one-stop-shop" model is shared by CVS Health (which owns Aetna insurance, Caremark PBM, CVS Pharmacy, and Minute Clinics), The Cigna Group (which owns Cigna Healthcare, Express Scripts PBM, Accredo specialty pharmacy, and MDLive telehealth), and UnitedHealth Group (which owns UnitedHealthcare insurance, OptumRx PBM, Optum Home Delivery, and OptumCare clinics).
Under this structure, the same entity that collects your monthly premium also decides which drugs are "preferred" and then directs you to receive care or prescriptions from the providers and pharmacies they own. This powerful trio currently controls the majority of prescriptions Americans. Critics argue this creates a massive conflict of interest, allowing these conglomerates to prioritize corporate profit over patient choice and health. When a middleman decides which medicine you can take and where you must buy it, they are inserting themselves directly into the private relationship between you and your doctor.

If you want to discover the specific mechanics and legal shields surrounding the most common hurdle used by these gatekeepers, explore my deep dive into The Permission Slip Trap: Decoding Prior Authorizations. To learn more about the administrative "speed bumps" designed to slow down your care, see my breakdown of utilization management tactics in The “No” That Isn’t Final
The Utilization Management "Speed Bumps"
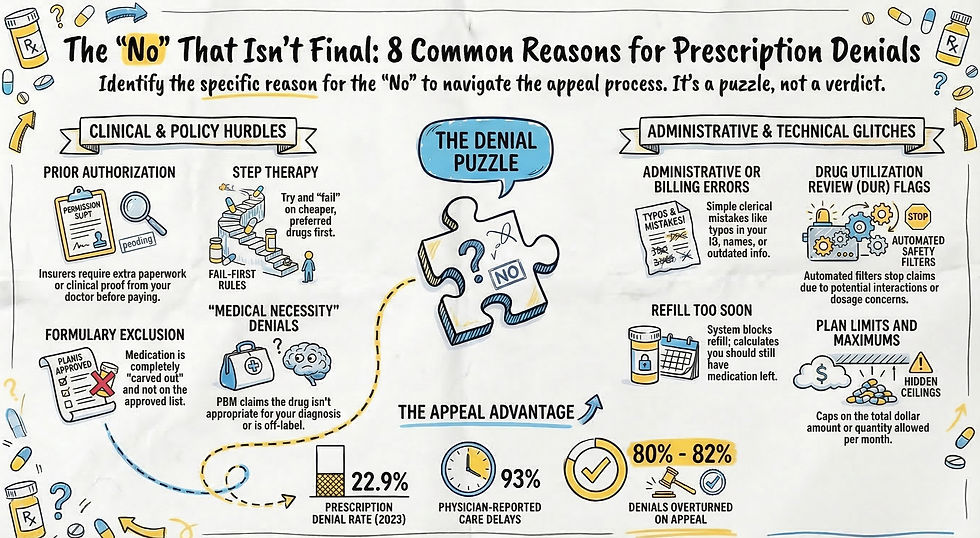
PBMs use several tools, collectively known as "Utilization Management," to control costs. While they claim these save money, for patients, they are administrative speed bumps designed to slow down your care:
Prior Authorization (PA): A "permission slip" where your doctor must prove to the PBM that you actually need the medicine before they agree to pay.
Step Therapy ("Fail-First"): A policy requiring you to try and "fail" on cheaper, preferred drugs before the PBM will cover the medication your doctor originally wanted.
Formularies: The master list of "approved" drugs.
Specialty Tiers: Moving life-saving drugs into a category where you are responsible for a much higher percentage of the cost.
The Staggering Burden on Your Care
This system places an enormous weight on the healthcare relationship. In Tennessee, doctors and their staff spend an average of 13 to 15 hours every week, nearly two full workdays, just filing the paperwork and phone calls required by PBMs. Nationally, the burden is even more shocking. According to a Gallup poll, Americans spend at least 12 million hours a week calling their health insurance companies to resolve issues. That is time and money that could be spent on more important things, but is instead swallowed by administrative hurdles.
These hurdles are a direct threat to your safety. The American Medical Association reports that 24% of physicians feel that these administrative delays have led to serious adverse events for a patient, including hospitalization or permanent impairment.
Reclaiming Your Power
The most important thing to remember is that a denial is not a final decision. It is just the beginning of negotiation, not the end of the road. Data shows that nearly 82% of prior authorization denials are overturned on appeal. The odds are in your favor, if you refuse to be the one who blinks first.
Knowledge is your strategic tool, and persistence is your primary weapon.
If you want to discover the specific mechanics of a winning Letter of Medical Necessity, explore The Ultimate Clinical Argument.



Comments